- 190 DD CCA, next to Jamia Mosque, DHA Phase 4 Sector CCA Dha Phase 4, Lahore, Punjab 54000, Pakistan
- 03-111-077-111
Vitiligo Treatment (Melanocyte transplant)
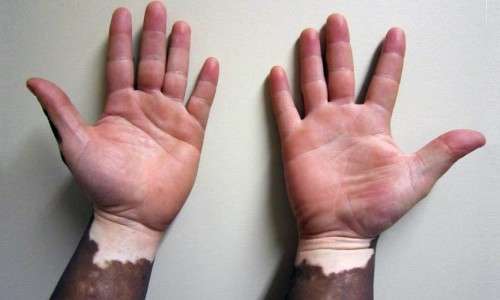
Q. What Is Vitiligo ?
In Indo-Pakistan region, Vitiligo is commonly known as (Phul-Behri) or Leukoderma.
Vitiligo (vit-ill-EYE-go) is a pigmentation disorder in which melanocytes (the cells that make pigment) in the skin are destroyed. As a result, white patches appear on the skin in different parts of the body. Similar patches also appear on both the mucous membranes (tissues that line the inside of the mouth and nose) and the retina (inner layer of the eyeball). The hair that grows on areas affected by vitiligo sometimes turns white.
Q. What is the cause of Vitiligo?
The cause of vitiligo is not known, but doctors and researchers have several different theories. There is strong evidence that people with vitiligo inherit genes that make them susceptible to depigmentation. The most widely accepted view is that the depigmentation occurs because vitiligo is an autoimmune disease—a disease in which a person’s immune system reacts against the body’s own organs or tissues. People’s bodies produce proteins called cytokines that, in vitiligo, alter their pigment-producing cells and cause these cells to die. Another theory is that melanocytes destroy themselves. Finally, some people have reported that a single event, such as sunburn or emotional distress, triggered vitiligo; however, these events have not been scientifically proven as causes of vitiligo.Q. Can milk, fish or other white foods if taken together cause vitiligo?
NO. Absolutely not. This myth exists only in India and Pakistan, where many believe that Vitiligo can be aggravated by eating fish or other white foods, or sour foods like citrus fruits; or by drinking milk shortly after eating fish. The reality is Vitiligo has not been shown to have any connection with diet nor does it have any impact on the severity of this condition. Many cuisines in various parts of the world cook fish in milk routinely. If this were true, all of them should have gotten vitiligo. To date no substantial scientific evidence has ever been given to support this myth.Q. Who Is Affected by Vitiligo?
About 0.5 to 1 percent of the world’s population have vitiligo. The average age of onset is in the mid-twenties, but it can appear at any age. The disorder affects both sexes and all races equally; however, it is more noticeable in people with dark skin. Vitiligo seems to be somewhat more common in people with certain autoimmune diseases, including hyperthyroidism (an overactive thyroid gland), adrenocortical insufficiency (the adrenal gland does not produce enough of the hormone called corticosteroid), alopecia areata (patches of baldness), and pernicious anemia (a low level of red blood cells caused by the failure of the body to absorb vitamin B12). Scientists do not know the reason for the association between vitiligo and these autoimmune diseases. However, most people with vitiligo have no other autoimmune disease. Vitiligo sometimes runs in families. Children whose parents have the disorder are more likely to develop vitiligo. However, most children will not get vitiligo even if a parent has it, and most people with vitiligo do not have a family history of the disorder.Q. What Are the Symptoms of Vitiligo?
People who develop vitiligo usually first notice white patches (depigmentation) on their skin. These patches are more commonly found on sun-exposed areas of the body, including the hands, feet, arms, face, and lips. Other common areas for white patches to appear are the armpits and groin and around the mouth, eyes, nostrils, navel, genitals, and rectum. Vitiligo generally appears in one of three patterns:- Focal pattern—depigmentation limited to one or only a few areas.
- Segmental pattern—depigmented patches that develop on one side of the body only.
- Generalized pattern—the most common pattern. Depigmentation occurs symmetrically on both sides of the body.
Q. Will the Depigmented Patches Spread?
Focal pattern vitiligo and segmental vitiligo remain localized to one part of the body and do not spread. There is no way to predict if generalized vitiligo will spread. For some people, the depigmented patches do not spread. The disorder is usually progressive, however, and over time the white patches will spread to other areas of the body. For some people, vitiligo spreads slowly, over many years. For other people, spreading occurs rapidly. Some people have reported additional depigmentation following periods of physical or emotional stress.Q. How Is Vitiligo Diagnosed?
The diagnosis of vitiligo is made based on a physical examination, medical history, and laboratory tests. A doctor will likely suspect vitiligo if you report (or the physical examination reveals) white patches of skin on the body, particularly on sun-exposed areas, including the hands, feet, arms, face, and lips. If vitiligo is suspected, the doctor will ask about your medical history. Important factors in the diagnosis include a family history of vitiligo; a rash, sunburn, or other skin trauma that occurred at the site of vitiligo before depigmentation started; stress or physical illness; and premature graying of the hair (usually before age 35). In addition, the doctor will ask whether you or anyone in your family has had any autoimmune diseases and whether you are very sensitive to the sun. To help confirm the diagnosis, the doctor may take a small sample (biopsy) of the affected skin to examine under a microscope. In vitiligo, the skin sample will usually show a complete absence of pigment-producing melanocytes. On the other hand, the presence of inflamed cells in the sample may suggest that another condition is responsible for the loss of pigmentation. Because vitiligo may be associated with pernicious anemia (a condition in which an insufficient amount of vitamin B12 is absorbed from the gastrointestinal tract) or hyperthyroidism (an overactive thyroid gland), the doctor may also take a blood sample to check the blood cell count and thyroid function. For some patients, the doctor may recommend an eye examination to check for uveitis (inflammation of part of the eye), which sometimes occurs with vitiligo. A blood test to look for the presence of antinuclear antibodies (a type of autoantibody) may also be done. This test helps determine if the patient has another autoimmune disease.Q. How Can People Cope With the Emotional and Psychological Aspects of Vitiligo?
Although vitiligo is usually not harmful medically, its emotional and psychological effects can be devastating. White patches of vitiligo can affect emotional and psychological well-being and self-esteem. People with vitiligo can experience emotional stress, particularly if the condition develops on visible areas of the body (such as the face, hands, arms, and feet) or on the genitals. Adolescents, who are often particularly concerned about their appearance, can be devastated by widespread vitiligo. Some people who have vitiligo feel embarrassed, ashamed, depressed, or worried about how others will react. Fortunately, there are several strategies to help people cope with vitiligo. Also, various treatments—discussed in the next section—can minimize, camouflage, or, in some cases, even eliminate white patches. First, it is important to find a doctor who is knowledgeable about the disorder and takes it seriously. You must let your doctor know if you are feeling depressed, because doctors and other mental health professionals can help people deal with depression. You should also learn as much as possible about the disorder and treatment choices so that you can participate in making important decisions about your medical care. Some people with vitiligo have found that cosmetics that cover the white patches improve their appearance and help them feel better about themselves. You may need to experiment with several brands of concealing cosmetics before finding the product that works best.Q: Is Vitiligo treatable?
Yes. In most of the cases vitiligo is a treatable disease, especially if diagnosed early and if the affected area is small.Q. What Treatment Options Are Available?
The main goal of treating vitiligo is to reduce the contrast in color between affected and unaffected skin. The choice of therapy depends on the number of white patches; their location, sizes, and how widespread they are; and what you prefer in terms of treatment. Each patient responds differently to therapy, and a particular treatment may not work for everyone. Current treatment options for vitiligo include medication, surgery, and adjunctive therapies (used along with surgical or medical treatments). Medical Therapies A number of medical therapies, most of which are applied topically, can reduce the appearance of vitiligo. These are some of the most commonly used:- Topical therapy. Creams, including corticosteroids, may be helpful in repigmenting (returning the color to) white patches, particularly if they are applied in the initial stages of the disease. Corticosteroids are a group of drugs similar to hormones such as cortisone, which are produced by the adrenal glands. Yet, as with any medication, these creams can cause side effects. For this reason, the doctor will monitor you closely for skin shrinkage and skin striae (streaks or lines on the skin).
- Light treatment. Light therapy or excimer laser treatments are also used to treat vitiligo, although results may not be permanent.
- Light Therapy / Phototherapy (PUVA & Narrow Band Ultra Violet B):
- Psoralen photochemotherapy also known as psoralen and ultraviolet A (PUVA) therapy, this is an effective treatment for many patients. The goal of PUVA therapy is to repigment the white patches. However, it is time consuming, and care must be taken to avoid side effects, which can sometimes be severe. Psoralen is a drug that contains chemicals that react with ultraviolet light to cause darkening of the skin. The treatment involves taking psoralen by mouth (orally) or applying it to the skin (topically). This is followed by carefully timed exposure to sunlight or to ultraviolet A (UVA) light that comes from a special lamp. You must minimize exposure to sunlight at other times.Known side effects of oral psoralen include sunburn, nausea and vomiting, itching, abnormal hair growth, and hyperpigmentation. Oral psoralen photochemotherapy may also increase the risk of skin cancer, although the risk is minimal at doses used for vitiligo. If you are undergoing oral PUVA therapy, you will be advised to apply sunscreen, avoid direct sunlight, and wear protective UVA sunglasses for a period of time after each treatment.
- Depigmentation. This treatment involves fading the rest of the skin on the body to match the areas that are already white. For people who have vitiligo on more than 50 percent of their bodies, depigmentation may be recommended. Patients apply the drug monobenzyl ether of hydroquinone (monobenzone) twice a day to pigmented areas until they match the already depigmented areas. You will be advised to avoid direct skin-to-skin contact with other people for at least 2 hours after applying the drug, as transfer of the drug may cause depigmentation of the other person’s skin. The major side effect of depigmentation therapy is inflammation (redness and swelling) of the skin. You may also experience itching or dry skin. Depigmentation tends to be permanent and is not easily reversed. In addition, a person who undergoes depigmentation will always be unusually sensitive to sunlight.Surgical TherapiesSurgical techniques may be an option when topical creams and light therapy do not work. These include:
- Autologous skin grafts. The doctor removes skin from one area of your body and attaches it to another area. This type of skin grafting is sometimes used for patients with small patches of vitiligo. The doctor removes sections of the normal, pigmented skin (donor sites) and places them on the depigmented areas (recipient sites). There are several possible complications of autologous skin grafting. Infections may occur at the donor or recipient sites. The recipient and donor sites may develop scarring, a cobblestone appearance, or a spotty pigmentation, or may fail to repigment at all. Many people find skin grafting neither acceptable nor affordable.
- Skin grafts using blisters. In this procedure, the doctor creates blisters on your pigmented skin by using heat, suction, or freezing cold. The tops of the blisters are then cut out and transplanted to a depigmented skin area. The risks of blister grafting include scarring and lack of repigmentation. However, there is less risk of scarring with this procedure than with other types of grafting.
- Micropigmentation (tattooing). This procedure involves implanting pigment into the skin with a special surgical instrument. It works best for the lip area, particularly in people with dark skin. However, it is difficult for the doctor to match perfectly the color of the skin of the surrounding area.The tattooed area will not change in color when exposed to sun, although the surrounding normal skin will. So even if the tattooed area matches the surrounding skin perfectly at first, it may not later on. Tattooing tends to fade over time. In addition, tattooing of the lips may lead to episodes of blister outbreaks caused by the herpes simplex virus.
- Autologous melanocyte transplants. In this procedure, the doctor takes a sample of your normal pigmented skin and places it in a laboratory dish containing a special cell culture solution to grow melanocytes. When the melanocytes in the culture solution have multiplied, the doctor transplants them to your depigmented skin patches. This procedure is currently experimental and is impractical for the routine care of people with vitiligo. It is also very expensive, and its side effects are not known.Additional TherapiesIn addition to medical and surgical therapies, there are many things you can do on your own to protect your skin, minimize the appearance of white patches, and cope with the emotional aspects of vitiligo:
- Sunscreens. People who have vitiligo, particularly those with fair skin, should minimize sun exposure and use a sunscreen that provides protection from both UVA and ultraviolet B light. Tanning makes the contrast between normal and depigmented skin more noticeable. Sunscreen helps protect the skin from sunburn and long-term damage.
- Cosmetics. Some patients with vitiligo cover depigmented patches with stains, makeup, or self-tanning lotions. These cosmetic products can be particularly effective for people whose vitiligo is limited to exposed areas of the body. Many cosmetic companies offer makeup or dyes that you may find helpful for covering up depigmented patches. Self-tanning lotions have an advantage over makeup in that the color will last for several days and will not come off with washing.
- Counseling and support groups. Many people with vitiligo find it helpful to get counseling from a mental health professional. People often find they can talk to their counselor about issues that are difficult to discuss with anyone else. A mental health counselor can also offer support and help in coping with vitiligo. In addition, it may be helpful to attend a vitiligo support group.
Q. When can the surgery be considered?
Surgical treatment should be considered for all those patients in whom the course of Vitiligo has not changed over a period of six months to one year and/or if the medical treatments/phototherapy did not render desired or routinely anticipated results. Best and most satisfactory results are seen in patients who have only a few small areas of vitiligo, and no new areas have developed in the last one to two years. Small and stable (not increasing in size) areas are the most successfully treatable areas with the melanocyte transplant.Q. What we do in our clinic Cosmetique for vitiligo patients?
1. Light Therapy / Phototherapy (PUVA & Narrow Band Ultra Violet B):A special kind of light with a specific wavelength and frequency is used to treat the affected area. The patient is given timed and controlled exposure to light in a special chamber. We use highly advanced machines by some of the finest brands in United States for PUVA and Narrow Band UVB therapy. Treatment with this special light is especially indicated if the area involved is too large to be handled with topical medicines or if the later has failed to regenerate colour in the area. Narrow Band UVB (NBUVB) therapy is the latest and highly recommended treatment available in the world today which now is available in our clinic in Pakistan as well.2. Melanocyte Transplant (The most advanced & latest method):In this very sophisticated method, the cells which make color (Melanocytes) are transferred from the normal skin to the diseased area. Once they are transferred, they start to make the color in the white diseased vitiligo area. It is a difficult method to learn for surgeon but is the most satisfying procedure for the patient, as it does not leave any scars and the results are amazing. Dr.Azim Jahangir Khan is the only dermatologist / cosmetic surgeon who is trained and licensed to perform this refined surgical technique in the country.
Q. Is the melanocyte transplant surgery painful?
No. The donor area (where the colour producing cells will be picked from) as well as the diseased/recipient area , both will be duly numbed with anesthetizing creams or injections using a very fine needle. All this ensures painlessness during the procedure.Q. Is general anesthesia required?
No. Only local anesthesia is used for vitiligo surgery. Patient is awake and talking throughout the procedure while not experiencing any discomfort or pain.Q. How long does the surgery take to perform?
It takes about 2-3 hours to perform this very delicate surgery.Q. What happens after the surgery?
Patient goes home with bandages on the donor (area from where the color producing cells were taken) was well as the recipient area (the diseased area of vitiligo). The bandages are taken off after about ten days. Patient can resume his daily activities in a couple of days.Q. When does the color starts to appear in the vitiligo area?
Usually it takes between 3 to 6 months for the color to appear in the melanocyte transplanted area.Q. How long does it take to see the full results?
It may take from 6 months to a year before the color can spread to the whole treated area. Remember, it takes some time for the tiny color producing cells to make color, so the patient has to be patient!Q. Would anyone be able to tell that I had the surgery done after a year or so?
Most likely not. It is sometimes difficult even for us to locate the exact spot where surgery was performed. Since stitches are not placed, scar is not visible. In some cases, the color may not match 100%, but it is so close to the surrounding skin that it is almost impossible to find out that the vitiligo ever existed there.Q. How much does the surgery cost?
It depends on the size of the treatment area. Vitiligo surgery usually starts from Rs. 40,000 (approx US$ 500) onwards. Please call our clinic or e-mail your photographs to get the exact estimate if needed. But the best way to know if you are an eligible candidate for vitiligo surgery would be to schedule a consultation with our doctor. After proper evaluation we will guide you about different treatment options and the most suitable treatment in your particular case.Q. Is Melanocyte Transplant Surgery commonly available in Pakistan and other countries?
No. Melanocyte Transplant Surgery is a very sophisticated surgery requiring very highly skilled doctors and very specialized equipment that is not available in most parts of the world. We are the only center in Pakistan providing Melanocyte Transplant Surgery. There are only a few places in the world, where Melanocyte Transplant Surgery is being performed and by the grace of God we are one of them.Q. What Research Is Being Conducted on Vitiligo?
In the past, research on the role that melanocytes play in vitiligo has greatly increased. Genetic advances have permitted relatively rapid increases in knowledge of melanocytes at the cellular and molecular levels. Much of the research that holds promise for understanding, treating, and possibly preventing vitiligo is supported by the NIAMS. Researchers are looking at the immune response to see if interrupting certain signals given off by melanocytes can help stop the spread of depigmentation. They are examining the way melanocytes receive signals from other skin cells that direct them to deposit the pigment. Others are trying to determine the molecular mechanisms involved in creating melanocytes. This understanding may allow researchers to stimulate the creation of melanocytes from stem cells of hair follicles and use them to add pigment back into affected skin. Such a therapy may be more effective and safer than current light therapies. The NIAMS also supports a large collaborative project looking for genes that may contribute to vitiligo in several ethnic groups. It is hoped that genetic analyses of these groups will enable identification of one or more vitiligo susceptibility genes and the roles the genes play in contributing to the disease. This work may lead to development of specific approaches to disease therapy and prevention for patients at high genetic risk.Melanocyte Transplant Procedure step by step In order to aide patients in understanding how the procedure is performed the team of dermatologists who specialize in this cutting edge treatment have broken the process into a series of steps. Your physician will also go over the procedure from start to finish with you during office visits. An unaffected area of the body is selected to take a small sample of skin. This area is called the “donor area.” The area is cleansed and numbed with several injections. A small piece of skin as thin as a sheet of paper is removed.
2. The donor skin is processed by our nurse. The nurse separates out the pigment producing cells, called melanocytes.
3. The area of vitiligo that will be treated is cleaned and numbed, similar to the donor area. This is the treatment area.
4. A dermabrader is used to remove only the very top layer of skin from the treatment area. A dermabrader is similar to an electric sander. You will hear a buzzing sound and feel pressure during this part of the procedure.
5. The melanocyte solution, made from your own melanocytes, is applied to this area.
6. The donor area and the treated area(s) are covered with a special dressing.
7. We ask that you stay in the Lahore area for 48 hours after the procedure, in case you need to be seen urgently.
8. You can resume all activities except for those which will cause the dressing to come off the treated area, such as showering or swimming.
9. After four to seven days (depending on the area treated), the dressing is removed in the dermatology clinic.
